Pill with imprint AHD 300 is Brown & Yellow, Capsule/Oblong and has been identified as Gabapentin 300 mg. It is supplied by ACI Healthcare USA, Inc.
Gabapentin is used in the treatment of Back Pain; Postherpetic Neuralgia; Epilepsy; Chronic Pain; Seizures and belongs to the drug class gamma-aminobutyric acid analogs. Risk cannot be ruled out during pregnancy. Gabapentin 300 mg is not a controlled substance under the Controlled Substances Act (CSA).

Gabapentin
- Imprint
- AHD 300
- Strength
- 300 mg
- Color
- Brown & Yellow
- Size
- 19.00 mm
- Shape
- Capsule/Oblong
- Availability
- Prescription only
- Drug Class
- Gamma-aminobutyric acid analogs
- Pregnancy Category
- C – Risk cannot be ruled out
- CSA Schedule
- Not a controlled drug
- Labeler / Supplier
- ACI Healthcare USA, Inc.
- Manufacturer
- Strides Shasun Limited
- National Drug Code (NDC)
- 71093-0121
- Inactive Ingredients
- corn starch, magnesium silicate, gelatin, titanium dioxide, ferrosoferric oxide, butyl alcohol, alcohol, isopropyl alcohol, potassium hydroxide, shellac, ferric oxide red, ferric oxide yellow, propylene glycol, ammonia
What is Gabapentin ?
Gabapentin is a medication used to treat seizures (epilepsy) and nerve pain (neuropathic pain). It belongs to a class of medications called anticonvulsants or antiepileptic drugs.
What does Gabapentin can do ?
- Seizure Management: Gabapentin may be used alongside other medications to reduce seizure frequency in adults and children aged three and older who experience partial-onset seizures.
- Postherpetic Neuralgia: In adults, gabapentin is effective for managing postherpetic neuralgia, which is persistent nerve pain following a Shingles infection.
- Horizant (Gabapentin Enacarbil): This long-acting prodrug of gabapentin is taken once daily, usually around 5 PM, to relieve restless legs syndrome (RLS) or nerve pain associated with postherpetic neuralgia.
- Generic Availability: Gabapentin is available in generic forms, though not all generics are interchangeable with some branded versions.
- Off-Label Uses: Gabapentin may also be prescribed off-label for conditions such as fibromyalgia, persistent hiccups, migraine prevention, and hot flashes. Different brands and formulations of gabapentin exist, each with specific uses and dosing instructions.
- Neurontin: Used to treat pain from shingles (postherpetic neuralgia) and, when combined with other seizure medications, treats partial-onset seizures in adults and children over three years old.
- Gralise: Specifically designed for treating postherpetic neuralgia and should not be used for other conditions.
- Horizant: An extended-release tablet intended for restless legs syndrome and postherpetic neuralgia.
- Generic Gabapentin Capsules: Used for treating postherpetic neuralgia and as an additional therapy for partial-onset seizures in adults and children over three years old.
Here’s a rundown of precautions, side effects, and how to take gabapentin:
Precautions:
- Allergies: Inform your doctor if you have any allergies to gabapentin or any other medications.
- Medical History: Disclose your medical history to your doctor, especially if you have a history of kidney disease, mood disorders (such as depression or bipolar disorder), substance abuse, or breathing problems.
- Pregnancy and Breastfeeding: Inform your doctor if you are pregnant, planning to become pregnant, or breastfeeding, as gabapentin may pose risks to the fetus or infant.
- Driving and Operating Machinery: Gabapentin may cause dizziness, drowsiness, or blurred vision, which can impair your ability to drive or operate machinery. Use caution when engaging in activities that require mental alertness until you know how gabapentin affects you.
- Alcohol and Sedatives: Avoid consuming alcohol or taking sedative medications while using gabapentin, as it can increase the risk of drowsiness and dizziness.
- Withdrawal: Do not stop taking gabapentin suddenly without consulting your doctor, as this can lead to withdrawal symptoms such as seizures, anxiety, insomnia, nausea, or sweating.
Side Effects:
Common side effects of gabapentin may include:
- Dizziness
- Drowsiness
- Fatigue
- Headache
- Nausea
- Blurred vision
- Dry mouth
- Weight gain
- Tremors
- Difficulty speaking
- Memory problems
Less common but more serious side effects may include:
- Suicidal thoughts or behavior
- Mood changes (such as depression or anxiety)
- Swelling of the hands, feet, or ankles
- Rapid weight gain
- Signs of infection (such as fever or sore throat)
- Unusual bruising or bleeding
- Severe skin reactions (such as rash, blistering, or peeling)
If you experience any severe or persistent side effects while taking gabapentin, contact your doctor immediately.
What Are the Risks of Taking Gabapentin ?
If you are between the ages of 18 and 60, take no other medications, and have no other medical conditions, you are more likely to experience the following side effects with gabapentin:
- Common Side Effects: Dizziness, drowsiness, tiredness, fever, and nystagmus (rapid, uncontrollable eye movements). Gabapentin-induced drowsiness can impair your ability to drive or operate machinery. Alcohol and other sedatives can enhance this effect.
- Behavioral Changes in Children: When used to treat epilepsy in children aged three to twelve, gabapentin may cause behavioral problems, hostility, aggression, or thought disturbances.
- Other Side Effects: Blurred vision, amblyopia (lazy eye), dry mouth, peripheral edema (fluid retention in feet and hands), tremor, sexual dysfunction, and gastrointestinal disturbances.
- Titration: Gabapentin should be titrated up slowly to reduce the risk of side effects, although this may delay the onset of its effects.
- Mental Health Risks: Similar to other anticonvulsants, gabapentin may increase the risk of depression and suicidal thoughts, especially in young adults under 24.
- Discontinuation Syndrome: Abruptly stopping gabapentin can cause withdrawal symptoms such as anxiety, insomnia, nausea, pain, and sweating. It should be tapered off slowly under medical supervision.
- Kidney Disease: The dosage needs to be reduced for individuals with kidney disease.
- Hypersensitivity Reactions: Rarely, hypersensitivity reactions can occur, including fever, rash, swollen lymph nodes, swollen facial features, or throat swelling.
- Drug Interactions: Gabapentin may interact with other medications, including antacids, hydrocodone, morphine, and other sedatives, potentially causing increased sedation or dizziness. It may also cause false-positive results on some urinary protein tests.
- Misuse and Abuse: There have been reports of gabapentin misuse and abuse, especially in individuals with a history of drug abuse.
- Administration: Gabapentin typically requires three times daily administration due to its short duration of effect. However, gabapentin enacarbil (brand name Horizant) is a long-acting prodrug that only requires once-daily dosing.
- Seizure Disorders: Gabapentin is only effective for partial-onset seizures and not for other types of seizure disorders.
- Interchangeability: Some branded and generic forms of gabapentin are not interchangeable.
Mechanism of Action
Gabapentin is a medication that is primarily used to treat epilepsy and neuropathic pain. Its exact mechanism of action is not fully understood, but it is known to interact with certain components of the nervous system. Gabapentin works primarily by binding to the α2δ subunit of voltage-gated calcium channels, which leads to a reduction in calcium influx and a subsequent decrease in the release of excitatory neurotransmitters. This action helps to stabilize neuronal activity and reduce symptoms of seizures and neuropathic pain. Although its exact mechanism is not fully understood, gabapentin’s effects on neurotransmission and neuronal excitability make it a valuable medication for a variety of neurological and pain-related conditions.
Here is a detailed explanation of the proposed mechanisms by which gabapentin exerts its therapeutic effects:
Mechanism of Action
- Binding to the α2δ Subunit of Voltage-Gated Calcium Channels:
- Gabapentin binds with high affinity to the α2δ subunit of voltage-gated calcium channels in the central nervous system.
- This binding inhibits the influx of calcium ions into neurons, which in turn reduces the release of excitatory neurotransmitters such as glutamate, norepinephrine, and substance P.
- By decreasing the release of these neurotransmitters, gabapentin helps to stabilize neuronal activity and reduce the hyperexcitability that contributes to seizures and neuropathic pain.
- Reduction of Excitatory Neurotransmission:
- The inhibition of calcium influx and subsequent reduction in neurotransmitter release results in decreased excitatory synaptic transmission.
- This reduction in excitatory signaling is believed to contribute to the anticonvulsant and analgesic effects of gabapentin.
- Modulation of GABAergic Neurotransmission:
- Although gabapentin is structurally similar to the neurotransmitter gamma-aminobutyric acid (GABA), it does not directly bind to GABA receptors or influence GABA synthesis or uptake.
- However, gabapentin may enhance the synthesis of GABA and increase its release in certain brain regions, which could contribute to its overall calming effect on neuronal activity.
- Inhibition of Central Sensitization:
- In conditions like neuropathic pain, there is often a phenomenon known as central sensitization, where the nervous system becomes sensitized to pain stimuli.
- By inhibiting calcium influx and reducing excitatory neurotransmitter release, gabapentin helps to diminish central sensitization and alleviate chronic pain symptoms.
Therapeutic Effects
- Anticonvulsant:
- Gabapentin’s ability to decrease neuronal excitability and stabilize electrical activity in the brain makes it effective in controlling seizures, particularly partial seizures.
- Analgesic:
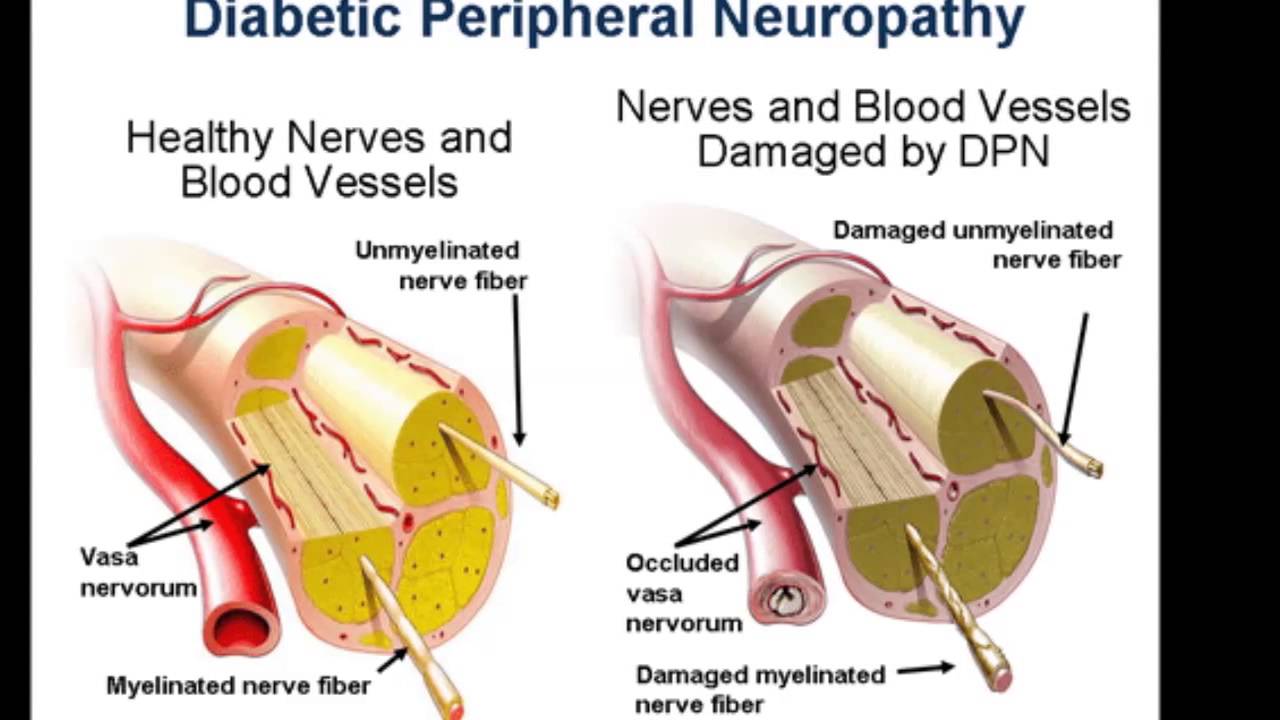
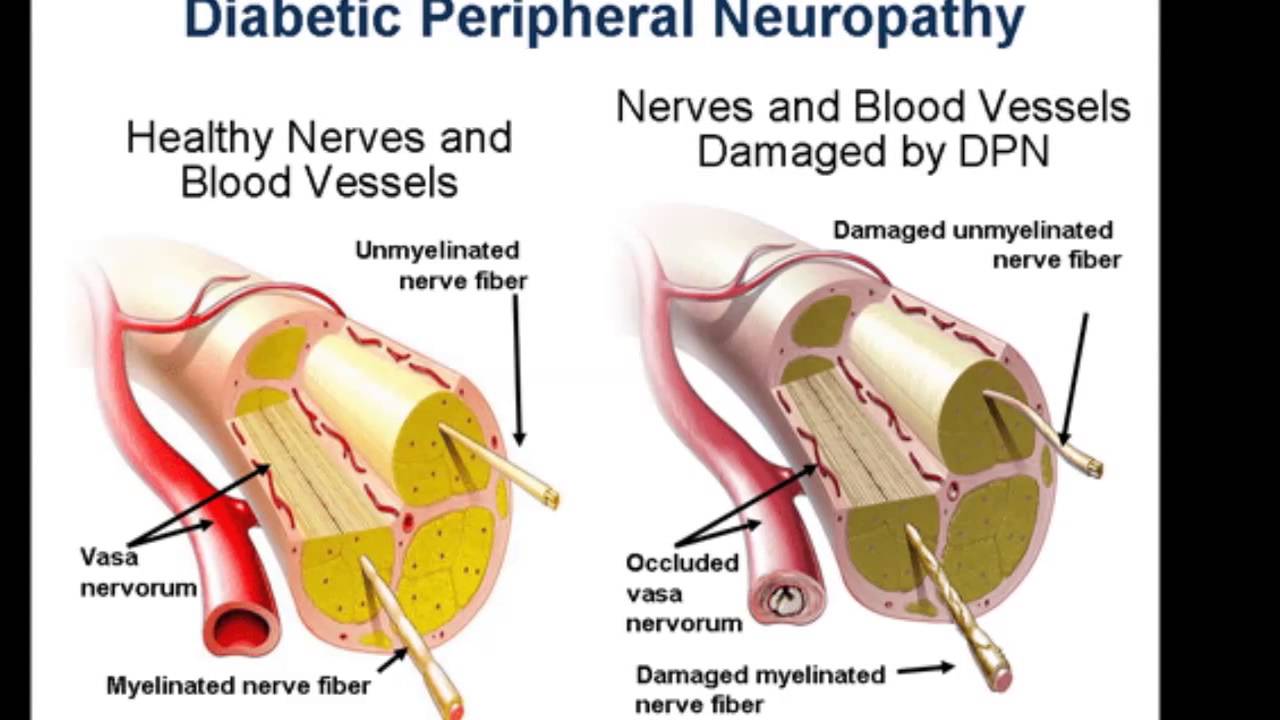
- The reduction in neurotransmitter release and inhibition of central sensitization make gabapentin effective in treating various forms of neuropathic pain, such as diabetic neuropathy and postherpetic neuralgia.
- Other Uses:
- Gabapentin is also used off-label for other conditions like restless legs syndrome (RLS) and certain anxiety disorders, where its modulatory effects on the nervous system can provide symptomatic relief.
How to Take Gabapentin:
- Dosage: Take gabapentin exactly as prescribed by your doctor. Do not adjust your dosage without consulting your doctor first.
- Administration: Gabapentin is usually taken orally with or without food. Swallow the capsule or tablet whole with a full glass of water.
- Timing: Take gabapentin at the same times each day to maintain a consistent level of the medication in your body.
- Gradual Dosing: If you are starting gabapentin treatment or increasing the dosage, your doctor may recommend starting with a low dose and gradually increasing it over time to minimize side effects.
- Duration of Treatment: Continue taking gabapentin for the full duration of treatment prescribed by your doctor, even if you start to feel better.
- Storage: Store gabapentin at room temperature away from moisture and heat. Keep it out of reach of children and pets.
Medications for Epilepsy
Epilepsy is a brain disorder involving recurrent seizures. Anti-seizure medications can help prevent or stop seizures. The choice depends on the type of seizure, the age of the person, the potential side effects of the medication, other medications they may be taking, or concurrent health conditions.
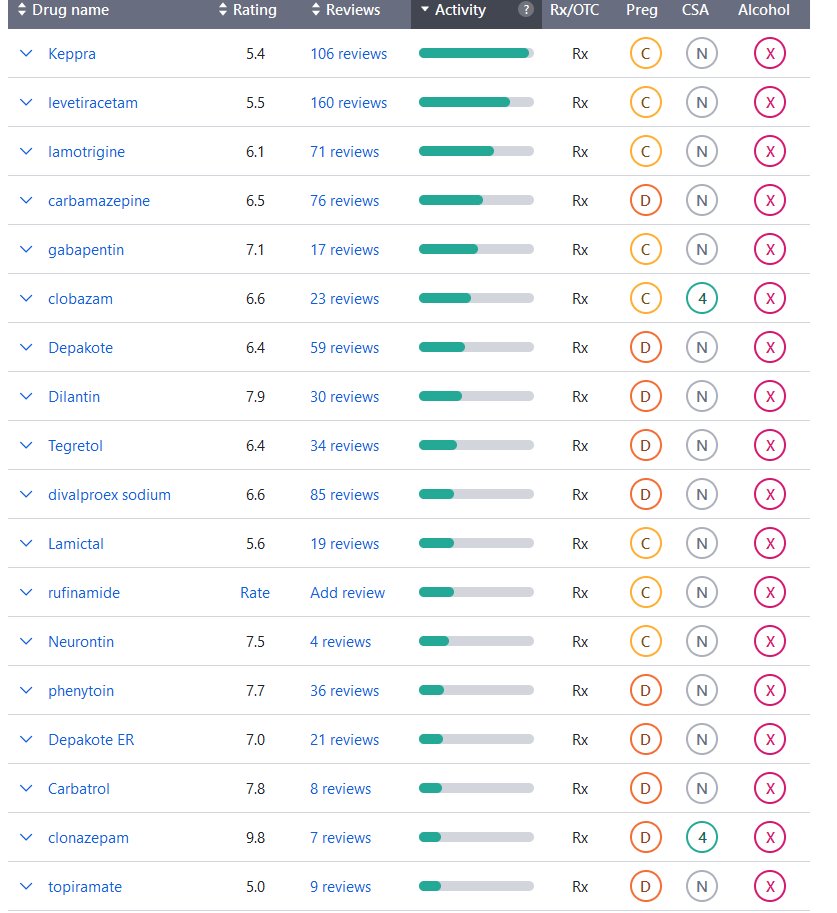
Various seizure types
- Acetazolamide (Diamox)
- Clobazam (Onfi)
- Clonazepam (Klonopin)
- Clorazepate (Tranxene)
Key Points of Taking Gabapentin
If you are between the ages of 18 and 60, take no other medications, and have no other medical conditions, you are more likely to experience the following side effects with gabapentin:
- Common Side Effects: Dizziness, drowsiness, tiredness, fever, and nystagmus (rapid, uncontrollable eye movements). Gabapentin-induced drowsiness can impair your ability to drive or operate machinery. Alcohol and other sedatives can enhance this effect.
- Behavioral Changes in Children: When used to treat epilepsy in children aged three to twelve, gabapentin may cause behavioral problems, hostility, aggression, or thought disturbances.
- Other Side Effects: Blurred vision, amblyopia (lazy eye), dry mouth, peripheral edema (fluid retention in feet and hands), tremor, sexual dysfunction, and gastrointestinal disturbances.
- Titration: Gabapentin should be titrated up slowly to reduce the risk of side effects, although this may delay the onset of its effects.
- Mental Health Risks: Similar to other anticonvulsants, gabapentin may increase the risk of depression and suicidal thoughts, especially in young adults under 24.
- Discontinuation Syndrome: Abruptly stopping gabapentin can cause withdrawal symptoms such as anxiety, insomnia, nausea, pain, and sweating. It should be tapered off slowly under medical supervision.
- Kidney Disease: The dosage needs to be reduced for individuals with kidney disease.
- Hypersensitivity Reactions: Rarely, hypersensitivity reactions can occur, including fever, rash, swollen lymph nodes, swollen facial features, or throat swelling.
- Drug Interactions: Gabapentin may interact with other medications, including antacids, hydrocodone, morphine, and other sedatives, potentially causing increased sedation or dizziness. It may also cause false-positive results on some urinary protein tests.
- Misuse and Abuse: There have been reports of gabapentin misuse and abuse, especially in individuals with a history of drug abuse.
- Administration: Gabapentin typically requires three times daily administration due to its short duration of effect. However, gabapentin enacarbil (brand name Horizant) is a long-acting prodrug that only requires once-daily dosing.
- Seizure Disorders: Gabapentin is only effective for partial-onset seizures and not for other types of seizure disorders.
- Interchangeability: Some branded and generic forms of gabapentin are not interchangeable.
Strides Shasun Limited
Strides Shasun Limited, now known as Strides Pharma Science Limited, is a global pharmaceutical company headquartered in Bangalore, India. The company specializes in the development, manufacture, and marketing of pharmaceutical products across various therapeutic segments. Here’s an overview of Strides Shasun Limited:
Company Overview
- Name and Headquarters:
- Current Name: Strides Pharma Science Limited (formerly Strides Shasun Limited).
- Headquarters: Bangalore, Karnataka, India.
- History and Evolution:
- Strides was founded in 1990.
- The company underwent several mergers and acquisitions, including the merger with Shasun Pharmaceuticals in 2014, leading to the name Strides Shasun Limited. In 2018, the company rebranded to Strides Pharma Science Limited.
Operations and Facilities
- Manufacturing:
- Strides operates multiple manufacturing facilities across the globe, including in India, the United States, and Europe. These facilities are designed to comply with international regulatory standards, including those of the U.S. Food and Drug Administration (FDA), the European Medicines Agency (EMA), and other regulatory bodies.
- The company’s manufacturing capabilities include a wide range of dosage forms such as tablets, capsules, injectables, topicals, and soft gels.
- Research and Development:
- Strides invests significantly in research and development to innovate and enhance its product portfolio. The R&D centers are equipped with advanced technology and staffed with experienced scientists who focus on developing complex generics and novel drug delivery systems.
Product Portfolio
- Generics:
- Strides Pharma Science produces a broad array of generic medications covering various therapeutic areas such as oncology, HIV/AIDS, immunosuppressants, antibiotics, and more.
- The company’s generic products are marketed globally, with a strong presence in the United States, Europe, and emerging markets.
- Specialty Pharmaceuticals:
- In addition to generics, Strides focuses on specialty pharmaceuticals, including niche and complex formulations that address unmet medical needs.
Key Areas of Operation
- Regulatory Compliance:
- Quality Assurance: Strides adheres to stringent quality control measures and regulatory requirements set by global health authorities.
- GMP Compliance: The company ensures that its manufacturing processes comply with Good Manufacturing Practices (GMP), ensuring the highest standards of product safety, efficacy, and quality.
- Market Strategy:
- Product Launches: Strides emphasizes the timely launch of generic medications to gain market share and provide cost-effective options to patients.
- Competitive Pricing: The company’s competitive pricing strategy makes its products accessible to a broad patient population.
- Global Partnerships:
- Strides collaborates with various global pharmaceutical companies to expand its market reach and enhance its product offerings.
Strategic Growth
- Acquisitions and Expansions:
- Strides has a history of strategic acquisitions and partnerships to strengthen its product portfolio and market presence.
- Recent expansions include acquiring new manufacturing facilities and entering into new markets to bolster its global footprint.
- Innovation:
- The company is committed to continuous innovation in pharmaceuticals, focusing on developing complex generics, biosimilars, and novel therapeutic solutions.
Corporate Responsibility
- Sustainability:
- Strides is committed to sustainable business practices, including efficient resource utilization, waste management, and reducing environmental impact.
- Community Engagement:
- The company engages in corporate social responsibility (CSR) initiatives aimed at improving healthcare access, supporting education, and contributing to the well-being of communities where it operates.
Conclusion
Strides Pharma Science Limited, formerly Strides Shasun Limited, is a prominent global pharmaceutical company known for its comprehensive range of generic and specialty pharmaceuticals. With a strong focus on quality, regulatory compliance, and innovation, Strides continues to expand its presence worldwide. The company’s commitment to sustainability and community engagement further underscores its role as a responsible and forward-thinking pharmaceutical provider.